Gibbs Reflective Cycle: 6 Steps to Better Reflection

Reflection is a key skill for learning from experiences and improving professional practice. The Gibbs Reflective Cycle, introduced in 1988, offers a structured six-step approach:
- Description: What happened? Focus on facts without analysis.
- Feelings: How did you feel before, during, and after? Understand emotional responses.
- Evaluation: What worked well? What didn’t? Identify strengths and weaknesses.
- Analysis: Why did things happen as they did? Explore causes and link to theory.
- Conclusion: What did you learn? Summarise key insights and areas for growth.
- Action Plan: What will you do differently? Set specific, measurable goals.
This cycle is widely used in healthcare for reflective practice and professional revalidation. It helps professionals connect theory to practice, enhance emotional awareness, and improve outcomes. Each step builds on the last, creating a continuous loop of learning and improvement.
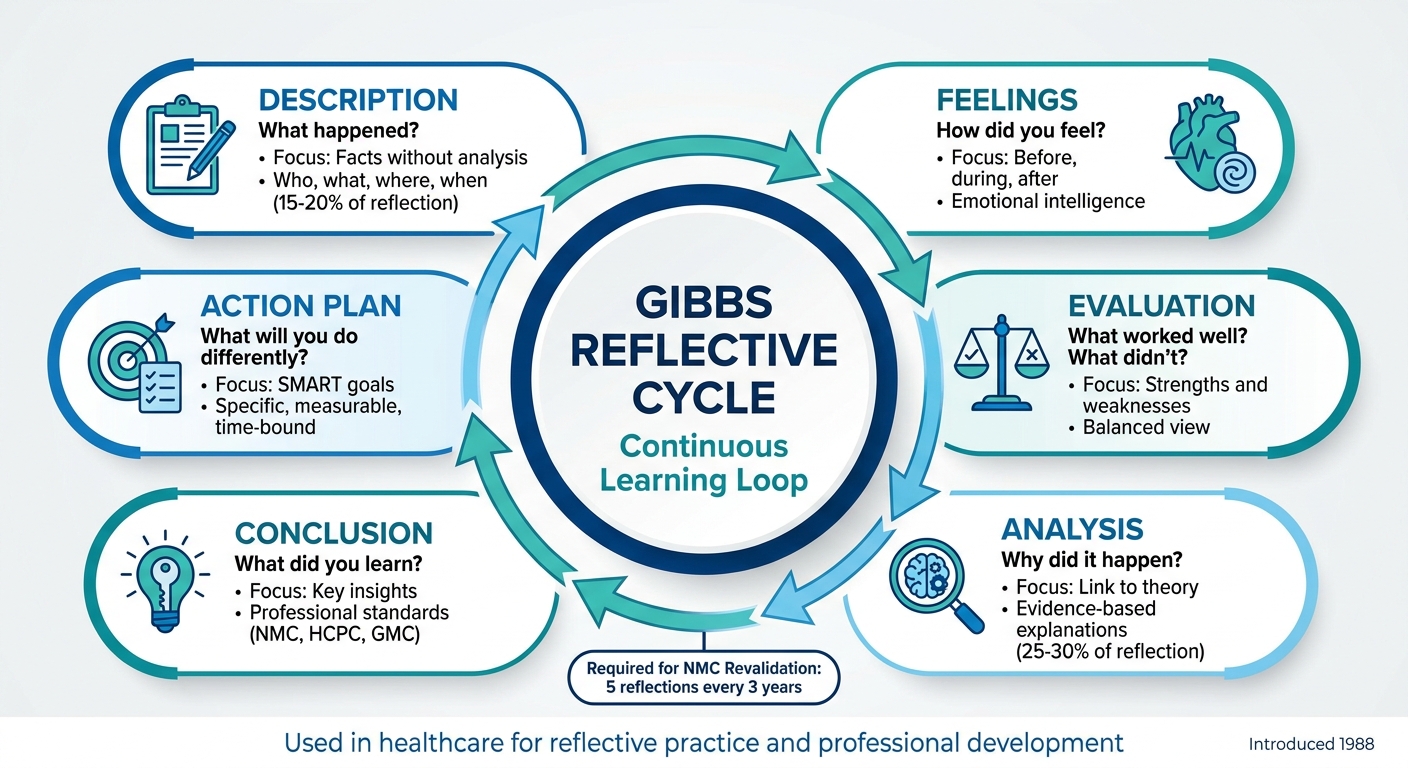
Gibbs Reflective Cycle 6 Steps for Healthcare Professionals
Gibbs Cycle tutorial- Writing reflections for nursing and midwifery students
sbb-itb-a476a38
Step 1: Description
The first step in Gibbs' six-part cycle is all about laying a solid foundation with a clear and factual description of the event. This step focuses on capturing the who, what, where, and when without diving into analysis or personal feelings.
"The goal is to record an objective, factual account of the event or experience without delving into analysis, interpretation or emotional input." - Simply Psychology
For healthcare professionals in the UK, organisations like the NMC, HCPC, and GMC emphasise the importance of precise descriptions when documenting CPD activities for revalidation purposes. So, how do you go about documenting the event effectively?
What Happened?
Begin by setting the context: when and where did the event occur? Was it during a ward handover, a clinical placement, or perhaps a team meeting? Then, identify who was involved. Even individuals who seemed to play a minor role could have had an impact on the situation.
Next, outline the sequence of events in the order they happened. What actions did you and others take? What was the initial goal or purpose of the activity? Finally, make a note of the immediate outcome - what happened as a result?
Establishing a clear and logical sequence is key before moving on to the next steps.
How to Write Clear and Factual Descriptions
Use neutral language to maintain objectivity. Instead of describing emotions like "angry" or "frustrated", focus on observable actions, such as "the patient raised their voice". Save any mention of feelings for Step 2.
The description should typically make up 15–20% of your total reflective essay. For example, in a 1,500-word reflection, aim for 225–300 words, or 300–400 words in a 2,000-word piece. A helpful tip is the "one-third rule": write your initial description, then review and cut it down by a third to ensure you're only including the most critical details.
"The single biggest mistake students make is spending 60% of their essay on Description, the stage worth the fewest marks." - Caleb S., Oxford University Graduate
Lastly, avoid circular logic. Don’t try to explain why things happened at this stage - that’s reserved for the Analysis step. Stick to the facts, and you’ll create a strong base for the rest of your reflection.
Step 2: Feelings
After documenting the facts, it's time to explore the emotional landscape of the experience. This step focuses on identifying your feelings before, during, and after the event - and understanding why those emotions are significant.
"This stage is crucial for developing emotional intelligence and understanding how emotions impact decision-making and actions." - Simply Psychology
Emotions are never neutral; they shape how we reason, communicate, and remain objective in professional settings. For example, a student midwife reflecting on a breastfeeding challenge described feeling a "surge of anxiety" and a "sense of helplessness" while observing a distressed mother. By acknowledging these emotions, she realised that her lack of clinical confidence was limiting her ability to offer emotional support. This insight led her to focus on improving mentorship and communication skills in her action plan.
Identifying Your Emotional Responses
Begin by noting your emotions at different stages of the event - before, during, and after. What was your initial reaction? Were you nervous, confident, frustrated, or perhaps relieved?
It's important to avoid the "objectivity trap", which dismisses strong emotions as unprofessional. For instance, a University of Edinburgh student reflecting on group work admitted feeling "guilty" when teammates had to cancel their evening plans to fix a shared mistake. This guilt motivated the student to "work harder in the evening and finish the task quicker", showing how emotions can drive positive changes in behaviour and commitment.
Instead of using vague terms like "sad" or "stressed", try to link your emotions to specific outcomes. Ask yourself: did anxiety arise from unfamiliarity with procedures? Did frustration affect your focus or motivation? Also, take a moment to consider how others involved might have been feeling - whether it’s the patient, their family, or your colleagues.
How Emotions Influenced Your Actions
The key to this step is understanding how your feelings shaped your behaviour. Emotions often make an event memorable, helping you connect what happened to why it turned out a certain way - whether positively or negatively.
"Reflection is not just a university requirement; it is a professional safeguard. The goal is to bridge the gap between clinical theory and safer patient outcomes." - Neelam Hussain, Senior NHS Sister
For healthcare professionals in the UK, reflecting on emotions plays a crucial role in meeting the "Prioritise People" and "Practise Effectively" domains of the NMC Code, as well as other professional standards. By recognising and validating all emotions - even those that feel negative or uncomfortable - you enable honest reflection without self-criticism. This awareness helps you identify personal triggers and patterns, improving self-regulation in future situations. Understanding your emotions not only sharpens clinical judgement but also supports compliance with standards from organisations like the NMC, HCPC, and GMC. This emotional insight lays the groundwork for assessing what went well and what could be improved.
Step 3: Evaluation
After exploring the emotions and details of the situation, it’s time to evaluate what worked well and what didn’t. The goal here is to pinpoint both the strengths and the areas that need improvement.
"To get the most out of your reflection focus on both the positive and the negative aspects of the situation, even if it was primarily one or the other." – University of Edinburgh
Striking a balance is essential. Even in situations that felt mostly negative, there are often elements that stood out as positive. Perhaps you handled a difficult moment with composure, or someone stepped in to offer support. On the other hand, even when things go smoothly, there’s usually room for fine-tuning.
At this stage, focus on what happened rather than why it happened. Save the deeper analysis for the next step. Ask yourself questions like: What went well? What contributed to the success? What could have been better? Taking this balanced approach will help you prepare for a more thorough exploration in the next stage.
What Went Well?
Start by identifying the positive aspects of the situation. Reflect on what contributed to success - whether it was your own actions, teamwork, or external factors. Did the initial goals get achieved? Were there specific behaviours, tools, or strategies that made a difference? Recognise the contributions of everyone involved, including yourself.
"This stage encourages a balanced view, acknowledging both achievements and areas needing improvement." – Hansani Bandara, Content Writer, Creately
For example, a student reflecting on a group project at the University of Edinburgh noted that dividing tasks based on individual strengths led to everyone meeting deadlines with high-quality work. However, the lack of a unified writing style created last-minute stress. In healthcare, examples might include effective communication from a patient, calm teamwork under pressure, or the successful use of clinical tools. Don’t forget to consider external factors, such as resources or policies, that helped things go smoothly.
What Could Have Been Better?
Next, look at the challenges or gaps. What didn’t go as planned? Was something missing that could have improved the outcome? Reflect on these aspects without being overly critical of yourself.
"Approach reflection with a growth mindset, viewing challenges as opportunities for learning rather than occasions for self-judgment." – Simply Psychology
Keep your evaluation balanced. While recognising what worked, also note areas where improvements could be made. Consider factors beyond your control, like limited resources or organisational constraints, to provide context and avoid taking full responsibility for negative outcomes. This balanced insight not only helps with personal development but also supports professional revalidation requirements.
Step 4: Analysis
Analysis is where you dig deeper, moving beyond describing what happened to critically examining why events unfolded the way they did.
"Analysis is where you shift from describing and evaluating the experience to critically examining why things unfolded the way they did." – Simply Psychology
Aim to allocate about 25–30% of your reflection to this stage. For a 1,500-word reflection, this means dedicating around 375 to 450 words. This section is your chance to connect what you experienced with professional standards, theoretical frameworks, and evidence-based practices, showcasing your ability to think critically.
Avoid falling into the trap of circular reasoning. Instead, back up your evaluations with solid, evidence-based explanations. For example, instead of saying, "Communication with the patient was poor", you might write: "The poor patient communication may be explained by communication anxiety in high-stakes clinical contexts, which Ley attributes to information overload combined with situational stress".
"Reflection is not just a university requirement; it is a professional safeguard. The goal is to bridge the gap between clinical theory and safer patient outcomes." – Neelam Hussain, Senior NHS Sister
Understanding the Causes and Context
Building on your evaluation, this is where you examine the underlying reasons behind what happened. Think about both internal factors (your own skills, assumptions, emotions, or knowledge gaps) and external factors (such as staffing levels, equipment availability, or the dynamics within the Multi-Disciplinary Team).
Ask yourself: Why did this happen? Were there alternative explanations? Consider the perspectives of everyone involved - your colleagues, patients, or even their families. For instance, if a handover didn’t go smoothly, was it because you were unfamiliar with the SBAR format? Or could it have been due to systemic issues like time constraints or insufficient staffing?
Looking at the broader picture can sometimes reveal that what seems like a personal shortcoming might actually reflect wider organisational challenges. For example, a breakdown in communication might not be about individual errors but could point to ineffective protocols between departments. This kind of insight sets the foundation for applying theoretical frameworks to your reflection.
Using Theoretical Frameworks
Integrating theory into your analysis helps tie your experiences to established evidence. This not only strengthens your reflection but also demonstrates a deeper understanding of professional practice. Link your experiences to frameworks, clinical guidelines (like NICE), or professional codes (such as the NMC Code).
Certain frameworks are particularly helpful for healthcare professionals. Carper’s Ways of Knowing, for instance, encourages you to analyse practice through empirical, ethical, personal, and aesthetic perspectives. Peplau’s Theory of Interpersonal Relations can shed light on the dynamics of nurse–patient relationships, while Benner’s Novice-to-Expert Model helps you understand your current competency level and why certain tasks might have been challenging. By applying these theories, you create a bridge between practice and evidence.
Use analytical language to connect theory to practice. Phrases like "This can be explained by…", "According to [Theory/Author]…", or "In light of [Professional Standard]…" can help you articulate your points. For instance, rather than simply stating that a patient felt comfortable because you were "good", link your actions to NMC Standard 1.1 and Kitwood’s Theory of Personhood to explain the outcome.
However, don’t just stop at quoting theories - critically evaluate whether they hold up in the realities of a busy hospital ward. This level of scrutiny is what elevates a basic reflection to a distinction-level one. By taking this approach, you not only improve your reflective practice but also ensure alignment with professional standards.
Step 5: Conclusion
Bringing everything together, the conclusion is where you synthesise your observations, emotions, and evaluations into clear, actionable insights.
"The Conclusion stage synthesizes the insights gained from all the previous stages." – Simply Psychology
This is your opportunity to pinpoint the specific skills or knowledge you've gained. Avoid vague statements like "I learned a lot." Instead, focus on the precise gaps you've identified and how they've been addressed. For example, you might realise that while you understood the clinical signs of sepsis, you lacked confidence in managing the situation under pressure. Or perhaps you’ve recognised that offering emotional support to distressed patients requires more than just empathy - it demands specific communication techniques that you need to develop. This kind of self-awareness highlights your commitment to professional growth.
Reflect on how your experience has shifted your assumptions. Maybe you previously thought that following clinical procedures was sufficient, but now you understand the importance of integrating technical tasks with person-centred care. Alternatively, you might have identified that what you saw as a personal shortcoming was actually a systemic issue - like poor handover protocols between departments - that requires organisational attention.
For revalidation purposes, clearly link your insights to professional standards, such as NMC Standard 1.1. The NMC mandates five written reflective accounts every three years, each demonstrating how your learning will influence your practice. By connecting your conclusions to standards like treating people with dignity and respect, you show how your reflection supports both your professional development and adherence to regulatory requirements.
Step 6: Action Plan
After drawing your conclusions, the next step is to transform those insights into actionable steps. This is where reflection becomes a professional commitment. As Neelam Hussain, Senior NHS Sister, aptly states:
"Without an Action Plan, a reflection is merely an observation".
For healthcare professionals in the UK, creating an action plan is a required step for revalidation with the NMC, GMC, and HCPC.
Your plan should go beyond broad statements like "I will improve my medication administration process". Instead, focus on specific actions, such as setting reminders, scheduling supervision, or establishing accountability measures. This approach ensures your intentions translate into measurable and meaningful changes.
Setting SMART Goals
To make your action plan effective, every goal should follow the SMART framework - Specific, Measurable, Achievable, Relevant, and Time-bound. This method turns general intentions into clear commitments. For instance, rather than saying, "I will communicate better with the team", you could specify: "Within the next 30 days, I will use the SBAR tool for every patient handover and seek feedback from my supervisor after three consecutive shifts".
Use this stage to target specific skills or knowledge gaps identified during your reflection. For example, if you’ve recognised uncertainty around IV medication administration, your goal might be: "Within the next month, I will complete the Trust's advanced IV medication administration module and request supervised practice for my next three administrations". Additionally, identify the resources you’ll need - whether it’s access to the RCN Library for updated protocols, shadowing a senior colleague, or attending a workshop.
Putting Your Action Plan into Practice
Once your SMART goals are defined, the next challenge is embedding them into your daily routine. Writing down your goals is only the start. Document your action plan in your professional portfolio, ensuring it contributes to the 35 hours of CPD required every three years. Discuss your plan during supervision to create accountability.
Set regular milestones to review your progress every six to twelve months, rather than waiting for revalidation deadlines. Keep track of completed activities such as workshop certificates, reflective notes from supervised practice, or colleague feedback, and store them in an easy-to-access location. Regular reviews will help ensure your action plan stays aligned with your current practice needs.
The action plan is the final step in the Gibbs Cycle, bridging one experience to the next and promoting continuous professional growth. By following this cyclical process, each reflection builds upon the last, creating a dynamic and ongoing pattern of improvement throughout your career.
Using Gibbs Reflective Cycle for NMC, HCPC, and GMC Revalidation
The Gibbs Reflective Cycle is a practical tool for meeting the revalidation requirements of UK healthcare regulators. For instance, NMC registrants are required to complete at least five written reflections within the three years leading up to revalidation. These reflections must be recorded using the NMC's designated reflective accounts form, and the Gibbs framework provides a structured approach to ensure compliance.
Each reflection must address key elements: what was learned, how practice improved, and how the experience aligns with the professional Code. The Royal College of Nursing highlights that "any reflective account needs to explain what you learnt from the CPD activity, feedback or experience; how you changed or improved your work as a result, and how this is relevant to the Code". The six stages of Gibbs' model facilitate this process by ensuring reflections are detailed, evidence-based, and focused on specific improvements.
Confidentiality is non-negotiable. To comply with the NMC Code 2018 and GDPR, reflections must be anonymised. This means using pseudonyms or labels like "Patient A" to avoid breaching confidentiality, which could result in a Fitness to Practise referral. Maintaining patient anonymity is a key aspect of ethical reflective practice, ensuring integrity in documentation. These written reflections also form the basis for the mandatory reflective discussion with another registrant from the same part of the register.
The Gibbs Reflective Cycle is equally relevant for HCPC and GMC revalidation. Both regulators emphasise reflective practice as part of CPD and appraisal processes to ensure professionals remain competent and continue learning from clinical experiences. The structured nature of Gibbs helps ensure reflections meet these standards while contributing to a comprehensive appraisal portfolio.
Here’s a breakdown of how each stage of the Gibbs Cycle aligns with practical revalidation needs:
| Gibbs Stage | Mapping to NMC Code Themes | Practical Application for Revalidation |
|---|---|---|
| Description | Promote Professionalism | Provide a factual account while maintaining patient anonymity. |
| Feelings | Prioritise People | Reflect on how emotions influenced the patient-provider relationship. |
| Evaluation | Preserve Safety | Examine what worked well and what didn’t, focusing on patient safety and outcomes. |
| Analysis | Practise Effectively | Connect the incident to evidence-based research and clinical guidelines. |
| Conclusion | Promote Professionalism | Summarise your learning and identify gaps in knowledge. |
| Action Plan | Practise Effectively | Outline specific CPD activities to address knowledge gaps. |
This structured approach ensures that each stage of the Gibbs Cycle contributes directly to meeting revalidation requirements while also supporting continuous professional development and improved clinical practice.
How Reflection Guide Simplifies Gibbs Reflective Writing
Reflection Guide makes structured reflection more manageable, even during hectic clinical schedules or revalidation periods. The platform provides guided templates aligned with the six stages of the Gibbs Reflective Cycle: Description, Feelings, Evaluation, Analysis, Conclusion, and Action Plan. Each stage includes tailored prompts, such as "What actually happened?" for Description or "Why did I feel this way?" for Feelings. These prompts help you stay objective and avoid blending analysis with factual accounts, a common challenge in reflective writing.
For healthcare professionals in the UK, the templates cater to the reflective accounts required for revalidation. The tool also accommodates the GPhC's four-stage cycle - Reflection, Planning, Action, and Evaluation - by adapting its structure accordingly.
In addition to structured templates, the platform incorporates privacy checks to safeguard patient confidentiality. These checks assist users in identifying and removing any identifiable information before finalising their reflections, ensuring compliance with professional privacy standards.
The platform also generates export-ready drafts suitable for portfolios, appraisals, and revalidation. These drafts provide a solid starting point for the mandatory reflective discussions with another registrant, as required by the NMC. Considering that around 2.5% of HCPC registrants (1 in 40) are randomly selected for CPD audits every two years, having compliant reflections ready to go can significantly reduce stress and save time during audits. By simplifying documentation and ensuring compliance, Reflection Guide supports healthcare professionals in maintaining high-quality reflective practices aligned with revalidation requirements.
Conclusion
The Gibbs Reflective Cycle offers a practical way to turn everyday clinical experiences into meaningful opportunities for growth. By working through its six stages - Description, Feelings, Evaluation, Analysis, Conclusion, and Action Plan - you go beyond simply recounting events. Instead, you gain a deeper understanding of why things happened and how to improve moving forward. This process strengthens the emotional awareness and clinical judgement needed for effective and safe patient care.
One of the model's greatest strengths is its cyclical nature, which allows you to revisit similar experiences over time. Rather than starting fresh with each reflection, you can build on prior insights. As the University of Edinburgh highlights, the model "lends itself particularly well to repeated experiences, allowing you to learn and plan from things that either went well or didn’t go well". This approach not only aids personal development but also ensures your reflections guide real improvements in practice.
When documenting experiences - whether it's a difficult conversation or a successful intervention - this structured approach ensures emotions are recognised and improvements are planned. The Action Plan stage is particularly important for revalidation, demonstrating to regulatory bodies like the NMC, HCPC, and GMC that your reflections lead to measurable changes in your practice.
To make the most of this reflective process, keep a journal and review experiences promptly. By honestly evaluating your strengths and areas for growth without harsh self-criticism, you’ll develop the self-awareness essential for delivering safe, evidence-based care. This habit doesn’t just meet regulatory requirements - it enhances the care you provide every day, ensuring both your patients and your professional practice benefit.
FAQs
How long should a Gibbs reflection be?
A Gibbs reflection needs to be detailed enough to cover all six stages effectively. Usually, this means writing a few sentences to a few paragraphs for each stage, depending on how deeply you need to reflect. The key is to offer meaningful insights while staying concise and aligned with your reflective purpose.
What’s the difference between evaluation and analysis?
In Gibbs' Reflective Cycle, evaluation focuses on identifying what went well and what didn’t, concentrating purely on the outcomes. It’s about assessing 'what' happened without delving into the reasons behind it. On the other hand, analysis digs deeper, exploring the underlying causes, the context, and the factors that influenced those outcomes. While evaluation provides a surface-level overview, analysis seeks to uncover the 'why', offering a more thorough understanding to guide future decisions.
How do I keep reflections confidential for revalidation?
To maintain confidentiality during revalidation, it’s important to use secure methods for recording your reflections. The official NMC template is a reliable option. Ensure these reflections are not shared publicly or with anyone who isn’t authorised to view them.
Keep your reflections safe by storing them securely. If you’re saving them digitally, make sure they are password-protected. For physical copies, use a locked storage location. These steps help protect the privacy of patients and colleagues while ensuring you meet professional standards.
