How to Get Into the Zone for Reflective Practice (And Why It Matters)

Reflective practice helps professionals, especially in healthcare, review their experiences to understand decisions and improve performance. It's not just a choice but often a regulatory requirement, like the NMC's revalidation process for nurses. The challenge lies in creating the right mindset and environment for effective reflection. Here's how you can make it work:
- Create a focused space: Eliminate distractions, find a quiet spot, and set clear boundaries to stay undisturbed.
- Time it right: Reflect soon after an event for accurate recollection. Short, consistent sessions work better than infrequent, long ones.
- Use a reflective model: Frameworks like Gibbs' Cycle or Driscoll's 'What?' model provide structure to organise thoughts and insights.
- Start small: Write one sentence a day or record quick voice notes to build a habit.
- Address barriers: Identify what's stopping you - time, emotions, or uncertainty - and adjust your approach accordingly.
Reflection isn't just about meeting requirements; it enhances patient care and personal growth. Begin by setting aside 30 minutes after a significant experience, choose a model, and write down your thoughts. Small, consistent efforts can lead to meaningful improvements in your practice.
5 Tips on Medical Reflections - how to improve your own practice!
sbb-itb-a476a38
Setting Up Your Space for Reflection
Your surroundings have a big impact on how well you can reflect. For healthcare professionals, interruptions occur as often as every two minutes, and each one raises the risk of error by 12.7%. The same goes for reflective practice - distractions can scatter your thoughts and make it harder to gain meaningful insights.
Removing Distractions
To focus, start by creating a "No Interruption Zone." Turn off your phone, close email tabs, and let others know you’re unavailable. Studies suggest our working memory can only handle about five key tasks at once, so even small distractions - like a buzzing phone or background noise - can break your concentration.
Physical boundaries are just as important. Pick a quiet, low-traffic spot and use clear signals to indicate you shouldn’t be disturbed. Gather everything you need - like your journal, pen, and any references - before you begin.
Once you’ve cleared distractions, set aside specific time slots to make reflective practice a regular habit.
Choosing the Right Time and Building Consistency
Timing plays a key role in effective reflection. The Royal College of Nursing advises, "the sooner you reflect on your activity, the more truthful to the event your recollection will be, so make it part of your regular routine". Ideally, carve out 30 minutes shortly after an experience to reflect. If writing immediately isn’t an option, record a voice memo and transcribe it later. To stay organised, set monthly reminders to review your portfolio and track recent learning moments.
What matters most is consistency, not duration. Short, regular sessions ensure reflection remains a priority instead of a last-minute task.
Taking Deliberate Pauses for Deeper Thinking
Reflection thrives when you step back from your usual tasks. These intentional pauses allow for what experts call "reflection-on-action" - a deeper look back at events to uncover lessons that might otherwise go unnoticed.
During these pauses, you can identify emotional responses, challenge assumptions, and link theory to practice. Even a quick, 6–7-minute writing session can bring out important insights. The trick is to make these pauses a natural part of your professional routine.
Choosing a Reflective Model to Guide Your Practice
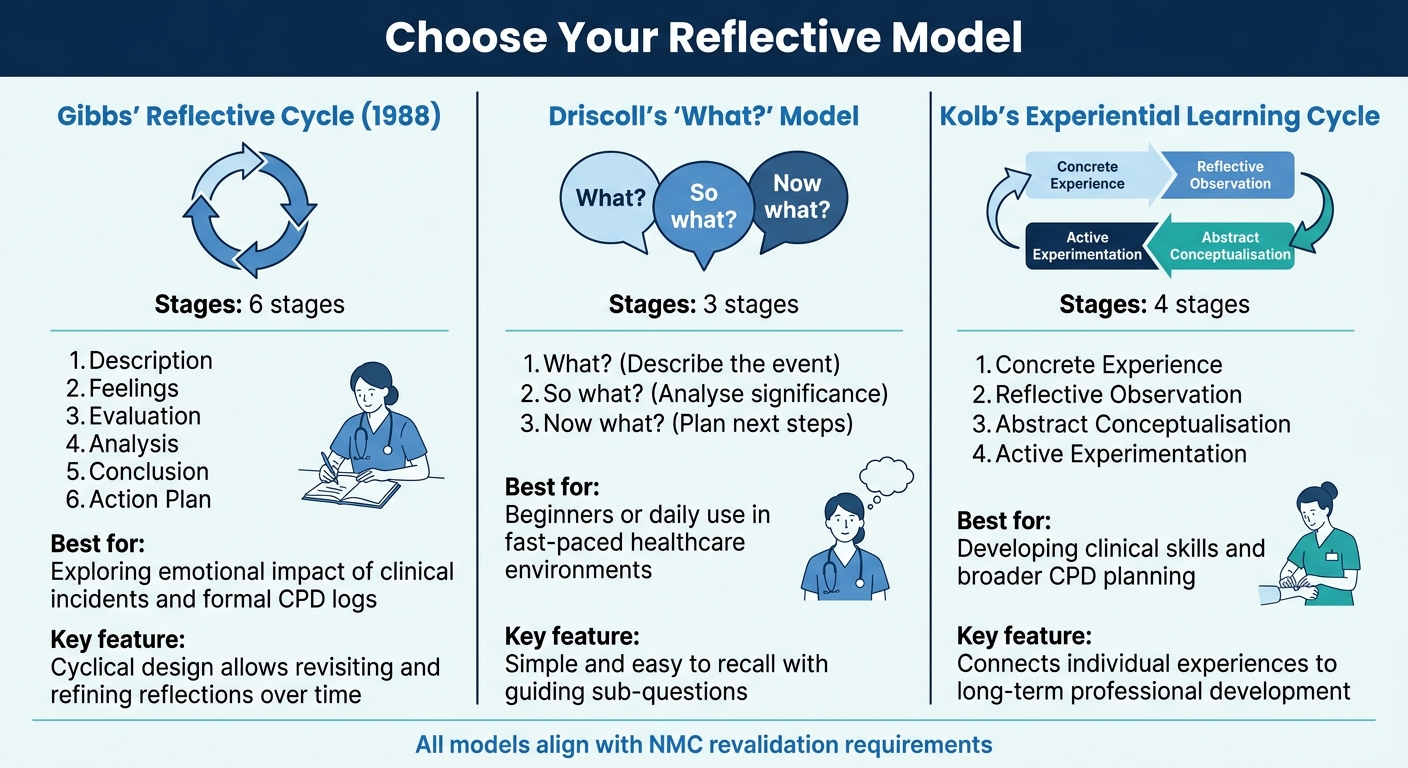
Comparison of Three Reflective Practice Models for Healthcare Professionals
Once you've set up a distraction-free space, the next step is selecting a reflective model that suits your needs. These models provide structure, helping you delve deeper into your experiences and organise your thoughts effectively. As the University of Southampton Library explains, "Think of a reflective model as a tool you can use to organise your thinking and structure your discussion of any insights that thinking leads to". Whether you're dealing with straightforward situations or more complex scenarios, reflective models - ranging from three-stage to six-stage frameworks - can adapt to your experience level.
These models are also aligned with professional standards, such as the NMC's revalidation requirements, which include five written reflections. Well-known options like Gibbs, Johns, and Driscoll are often recommended for meeting these standards. However, it’s important to view these models as flexible guides, not strict rules. If one doesn’t work for a particular situation, feel free to try another. The key is to choose a model that matches the complexity of your experience, ensuring your reflective practice remains effective and smooth.
Gibbs' Reflective Cycle
Gibbs' Reflective Cycle (1988) breaks reflection into six stages: Description, Feelings, Evaluation, Analysis, Conclusion, and Action Plan.
This model is particularly helpful when you want to explore the emotional impact of an event, such as a clinical incident, or when writing formal CPD logs. The "Feelings" stage encourages you to examine how emotions influenced your actions, offering valuable insight - especially in challenging situations. Its cyclical design allows you to revisit and refine your reflections over time, making it an excellent tool for ongoing learning.
Driscoll's 'What?' Model
If you're just starting with reflective practice or need a straightforward framework for daily use, Driscoll's 'What?' Model might be the right choice. It’s based on three simple questions: "What?" (describe the event), "So what?" (analyse its significance), and "Now what?" (plan your next steps).
This model’s simplicity makes it easy to recall, even in the fast-paced environment of healthcare. By incorporating guiding sub-questions - like "What was my role?" or "What influenced my decisions?" - you can ensure your reflection goes beyond surface-level observations and provides meaningful insights.
Kolb's Experiential Learning Cycle
Kolb's Experiential Learning Cycle offers another approach, focusing on four stages: Concrete Experience, Reflective Observation, Abstract Conceptualisation, and Active Experimentation. This model is ideal for turning practical experiences into ongoing professional growth.
Kolb's cycle works well when you're aiming to develop specific clinical skills or refine techniques based on what you've learned. Often used for broader CPD planning, it connects individual experiences to long-term professional development, ensuring that each encounter contributes to your growth as a practitioner.
Developing a Writing Habit for Reflection
Once you've chosen a structured model for reflection, the next step is turning it into a daily habit. With busy work schedules and personal responsibilities, finding time for reflective writing can feel like a challenge. But the key lies in consistency, not lengthy writing sessions. Regular practice strengthens the reflective process and supports continuous professional development (CPD) and revalidation.
Starting with One Sentence a Day
Facing a blank page can be daunting, but meaningful reflection doesn’t require pages of writing. Start small - commit to writing just one sentence each day that captures a key moment or thought. This simple, low-pressure approach helps you build momentum without feeling overwhelmed.
When you have more time, try the six-minute rule: write non-stop for six minutes about a specific event or experience. Don’t pause to edit or worry about grammar - just let your thoughts flow freely. As Janet Hayes-Hall, Clinical Dental Adviser at the General Dental Council, explains:
Writing is a private process and takes longer, allowing greater and deeper thought processes.
This method encourages uncensored thinking, helping you tap into deeper reflections.
If writing still feels difficult, consider recording voice notes immediately after an event and transcribing them later. Setting digital reminders can also nudge you to jot down quick reflections, making it easier to integrate the habit into your daily routine. Over time, even brief entries can reveal valuable insights and patterns.
Spotting Patterns Through Regular Writing
The true power of reflective writing often becomes apparent over time as recurring themes start to emerge. Reviewing your entries regularly - whether monthly or before an appraisal - can help you identify trends, such as repeated challenges, newly acquired skills, or areas where further learning is needed. Use the Relating stage of reflection to connect current experiences with past ones. Ask questions like, "Have I encountered this before?" or "What similarities exist between these situations?" These insights not only guide your professional development but also enhance your day-to-day practice and long-term growth, aligning with revalidation requirements.
Examining Beliefs That Hold You Back
One of the most impactful aspects of reflective writing is its ability to uncover assumptions or beliefs you might not realise you hold. Stephen Brookfield refers to these as "taken-for-granted" assumptions - unconscious thoughts or biases that could be hindering your professional growth.
Go beyond merely recounting events and dig deeper into the why. Ask yourself, "What was I thinking at the time?" or "What shaped my decisions in that moment?". This kind of critical questioning can bring hidden biases or habitual thought patterns to light - ones that may not be serving you or your patients. The goal isn’t to be overly critical of yourself but to approach these discoveries with honesty and a willingness to learn. By identifying and challenging these limiting beliefs, you create opportunities to improve both your practice and the care you provide to patients.
Getting Past Common Barriers to Reflection
Overcoming obstacles is crucial for maintaining a consistent and meaningful reflective practice, which plays an essential role in professional growth and revalidation. Common barriers include lack of time, emotional discomfort, and procrastination.
The first step is recognising when and why you might be avoiding reflection. Is it the act of writing itself, the emotional weight of certain experiences, or simply not knowing where to start? Once you've identified the issue, tailor your approach: if expressing emotions feels difficult, try using visual tools like mind maps or fishbone diagrams to organise your thoughts. Below, you'll find ways to reframe stress and push yourself beyond your comfort zone.
Viewing Stress as a Learning Opportunity
Stressful situations, while tough to revisit, can hold valuable lessons. Reflection allows you to break down what happened and understand why. As Brian Lucas, Associate Lecturer at The Open University, notes:
Reflection is a vital element of nursing practice and has a wide-ranging purpose including... recognition of emotional responses to care situations and exploring wider issues, such as healthcare culture.
When reflecting on a challenging event, go beyond simply recounting the details - focus on your emotional responses and the broader context. For example, consider whether gaps in team training or practice policies contributed to the situation. This kind of root cause analysis turns stress into actionable insights. Paul Russell-Roberts from RCNi highlights that "Learning does not require excellence – small, consistent steps, such as micro-learning, on-the-go reflection and compassionate pacing are key". Even dedicating six or seven minutes to free writing about a stressful incident can help you process emotions and pinpoint areas for improvement.
Once you've reframed stress in this way, you'll be better prepared to push beyond your comfort zone and deepen your reflective practice.
Pushing Beyond Your Comfort Zone
Reflective practice can also reveal when you've become too comfortable. If you're avoiding certain types of reflection or sticking to familiar, surface-level topics, it might be time to challenge yourself. Ask deeper questions like: "What assumptions am I holding onto?" or "What emotions am I hesitant to explore?".
If reflecting feels isolating, try collaborative approaches such as clinical supervision or group discussions. Hearing others' perspectives on an incident can highlight blind spots and lighten the emotional load of reflecting alone. Additionally, balancing reflections on positive experiences with challenging ones can reduce stress and help you appreciate your growth. The Royal College of Nursing advises: "The sooner you reflect on your activity, the more truthful to the event your recollection will be, so make it part of your regular routine".
Maintaining Reflective Practice Over Time
Sustaining reflective practice involves making it a natural part of your professional routine rather than an occasional activity. When reflection becomes second nature, it not only supports your immediate learning but also helps you meet long-term regulatory expectations.
Making Reflection Part of Your Daily Routine
Reflecting soon after an event helps capture details while they’re still fresh. If you’re short on time, try recording a quick voice note and expand on it later. Keep things interesting by using different methods like sketches, word clouds, or short discussions. You can also weave reflection into your existing professional activities, such as team meetings or annual appraisals. Setting a monthly reminder to update your portfolio ensures consistency, and having a copy of the NMC Code on hand makes it easier to connect your reflections to professional standards. By making reflection a daily habit, you create a foundation for reviewing your growth over time.
Looking Back to See Your Progress
Once you’ve established a regular reflection routine, take time to review your portfolio periodically. During your annual appraisal, revisit your entries to identify patterns, recurring themes, or areas where you’ve grown. Organising your portfolio monthly can help you avoid last-minute stress and ensures it includes a balanced mix of challenges and achievements. As the Royal College of Nursing points out, "Not all change happens overnight – some of the areas of development you identify might need further work – this is fine. What matters is that you are able to demonstrate evidence of recognising the impact of the Code".
Using Reflection for Revalidation and CPD
For NMC revalidation, you’ll need at least five written reflective accounts completed within the three years leading up to your revalidation date. Use the NMC’s approved form to document each reflection, detailing what you learned, how your practice has evolved, and how the experience aligns with the Code. These reflections can draw on CPD activities, feedback, or significant professional events, but must protect the anonymity of patients and colleagues. Spread your reflective activities evenly across the three-year cycle to avoid a last-minute rush. This consistent approach not only meets regulatory requirements but also strengthens your professional development. Tools like Reflection Guide can help you structure your entries with recognised models and built-in privacy features. As La Trobe University aptly states, "Reflective practice is a tool that will help you to remain an active, mindful and learning practitioner".
Conclusion
Reflective practice isn’t just about meeting professional requirements - it’s a way to improve patient care and grow as a healthcare professional. A study from the First Affiliated Hospital of Nanchang University, conducted between September 2021 and September 2023 with 97 nursing interns, highlights this. It found that those trained in reflective practice scored higher in compassion experience (P=0.040), sympathetic understanding (P=0.045), and the ability to empathise with others (P=0.025) compared to those who didn’t engage in reflection. These skills directly contribute to stronger patient connections and better care.
The evidence makes a strong case for adopting reflective practices. Whether it’s creating a quiet space to reflect, using tools like Gibbs' Reflective Cycle, or jotting down quick notes after a shift, the key is consistency. Even small actions, like writing one sentence a day or using visual aids like fishbone diagrams, can help build a lasting habit. As Margaret Codd, Quality Improvement Facilitator at the Health Service Executive, puts it:
Reflective practice is essential if we are to learn from what's happened to develop and improve not only our future practice, but our personal and professional wellbeing too.
Reflection doesn’t just tick the box for NMC revalidation; it also helps prevent the risk of professional stagnation. La Trobe University warns:
Any professional skill can become routine and unconscious, but stagnancy can be dangerous in a complex, specialised and rapidly changing profession like healthcare.
Making reflection part of your daily routine enhances your professional standards and enriches your interactions with patients. Start small - set aside 30 minutes of uninterrupted time to reflect on a patient experience, apply a reflective model, and document your thoughts. This simple commitment can have a profound impact on both your practice and your career. Every moment spent reflecting is an investment in better care and personal growth.
FAQs
Which reflective model should I use?
Gibbs' Reflective Cycle is a well-regarded tool for structured reflection. It breaks the process into six stages: description, feelings, evaluation, analysis, conclusion, and action planning. This step-by-step approach is especially useful for healthcare professionals, as it supports clinical reflective practice and encourages deeper understanding and professional development.
How can I reflect when I’m too busy?
If finding time to reflect feels challenging, there are simple ways to fit it into your day. Use your phone to record voice notes while the experience is still fresh, and transcribe them when you have more time. Take advantage of short breaks, like the moments between tasks or at the end of your workday, to note down key takeaways. Even a few minutes of regular reflection can make a big difference in supporting your professional development.
What counts as a good reflection for NMC revalidation?
A strong reflection for NMC revalidation should centre on actual experiences from your professional practice. These might include Continuing Professional Development (CPD) activities, feedback you've received, or particular events you've encountered in your role. It's important to clearly explain what you learned from these experiences, how they have helped enhance your practice, and how they align with the principles outlined in the NMC Code.
Your reflection should be honest and thoughtful, offering genuine insight into your professional growth. Make sure to record it on the approved NMC form and, if necessary, discuss it with another NMC registrant who can review and sign it off.
