Reflective Practice Is Not a Task: Why It Matters for Learning and Wellbeing

Reflective practice isn’t just about meeting professional requirements; it’s a structured way to learn from your experiences and improve both your skills and emotional wellbeing. It helps healthcare professionals evaluate their actions, decisions, and emotions systematically, leading to better patient care and personal growth. However, the key is purposeful reflection, not just ticking boxes.
Key Takeaways:
- What it is: A structured process for analysing workplace experiences to learn and grow.
- Why it matters: Enhances clinical skills, builds emotional resilience, and improves patient outcomes.
- How to do it: Use models like Gibbs, Driscoll, or Kolb for structured reflection. Dedicate 15–20 minutes daily or use tools like reflective journals or apps.
- Challenges: Time constraints, workplace support, and emotional barriers can make it hard, but consistency and support systems help.
Start small: Reflect daily on what went well, what didn’t, and how you can improve. Use these insights to grow professionally and personally.
How Reflective Practice Improves Learning and Wellbeing
Building Professional Skills and Knowledge
Reflection turns everyday clinical experiences into intentional opportunities for professional growth. It helps identify areas where skills can be improved and new knowledge can be gained. As Fiona Barchard, Curriculum and Programme Lead at the University of Northampton, explains:
"The application of reflection to practice has clear advantages, for example it enables nurses to learn from clinical events and adapt and enhance their skills."
By engaging in reflection-on-action - where incidents are analysed after they occur - healthcare professionals can uncover specific lessons and pinpoint areas for development. This process not only strengthens clinical judgement but also fosters a deeper emotional understanding. Margaret Codd, Quality Improvement Facilitator at the Health Service Executive, highlights:
"Dedicated space for reflection has the capacity to open creative and critical insight for individuals to turn ad hoc learning and experience into deeper knowledge."
Recording reflections not only satisfies regulatory requirements but also provides a tangible way to track professional progress over time. Beyond improving technical skills, structured reflection plays a key role in building emotional resilience, which is essential in high-pressure clinical settings.
Reducing Stress and Building Resilience
Reflection serves as a much-needed opportunity to process difficult experiences and understand emotional responses, helping to alleviate the weight of stress. Margaret Codd underscores the importance of this practice:
"Reflective practice is essential if we are to learn from what's happened to develop and improve not only our future practice, but our personal and professional wellbeing too."
In December 2021, the Health Foundation and the Q community hosted a Person-Centred Healing Workshop for 140 healthcare workers. Facilitated by Margaret Codd and her team, the session adapted a small-group reflective model for a large-scale digital format. Using chat functions, participants shared stories from the COVID-19 pandemic, creating a space for "deep listening" and collective emotional processing. The workshop was described as a "highly rewarding and healing experience" that helped staff navigate challenging experiences and build resilience. As Codd observed:
"The narrative of each person in the team contributed to a nuanced, collective story that helped to bridge understanding, widen perspectives, and inspire fresh empathy across the whole of the team."
Research Evidence for Better Patient Care
Reflective practices have a direct link to improving patient care. Brian Lucas, Associate Lecturer at The Open University, emphasises:
"The ability to reflect on, and learn from, practice experiences is essential for nurses when seeking to provide effective person-centred care."
Becky Ingham-Broomfield supports this view, noting:
"Reflection enables nurses to learn from their experiences and incorporate that learning into practice, with the ultimate aim of improving patient care."
sbb-itb-a476a38
The Benefits of Reflective Practice
Reflective Models for Healthcare Professionals
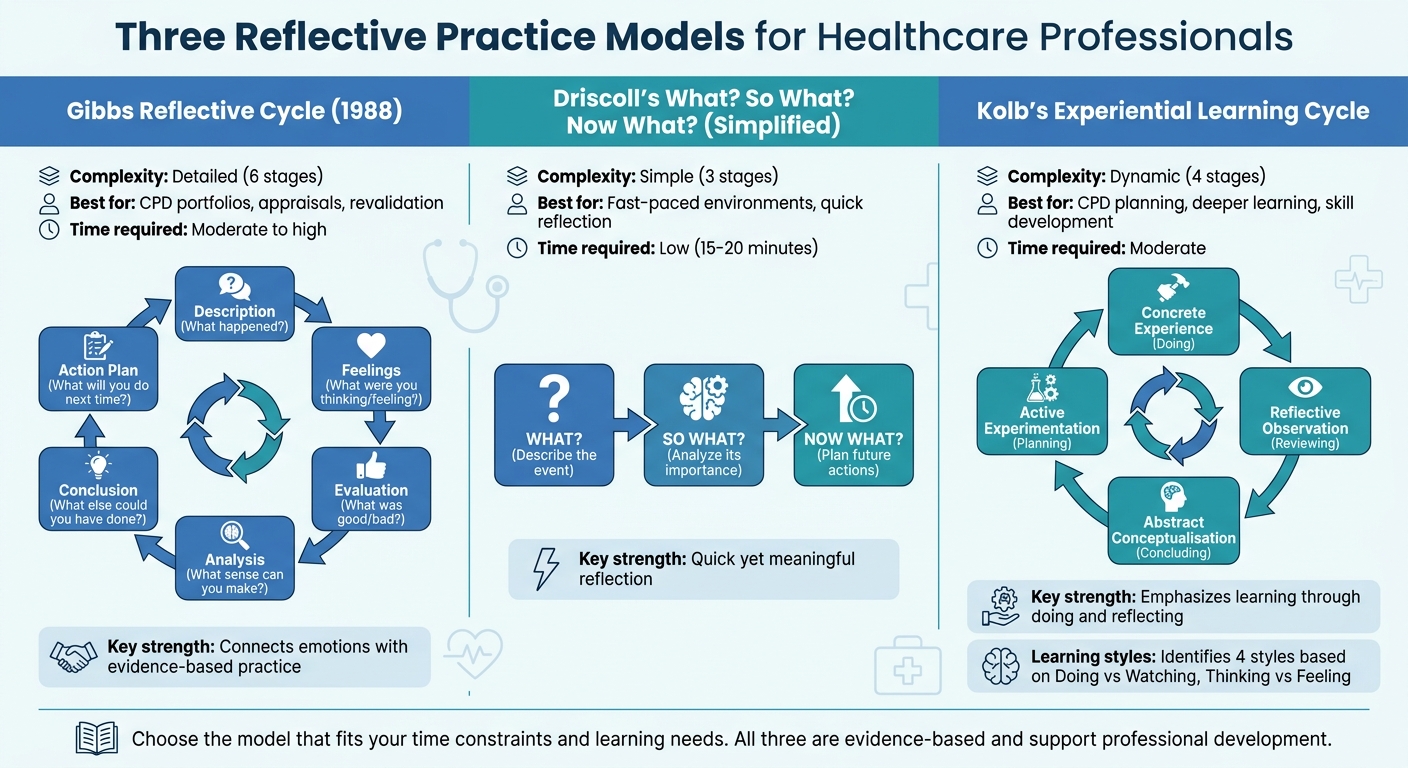
Three Reflective Practice Models for Healthcare Professionals: Gibbs, Driscoll, and Kolb
Structured reflection turns abstract experiences into valuable lessons. In healthcare, three models stand out for their practical use: Gibbs Reflective Cycle, Driscoll's What? So What? Now What?, and Kolb's Experiential Learning Cycle. Each model caters to different needs, depending on the complexity of the situation and the time available.
Gibbs Reflective Cycle
Graham Gibbs introduced this model in 1988, offering a six-stage framework for analysing clinical experiences. The stages - Description, Feelings, Evaluation, Analysis, Conclusion, and Action Plan - create a continuous cycle where each experience informs future actions.
This model encourages healthcare professionals to recognise the emotional aspects of their decisions. The "Analysis" stage connects practical experiences with academic research, clinical guidelines, or evidence-based practices. The University of Edinburgh Reflection Toolkit highlights its value:
"By thinking about each stage you are more likely to engage critically with your learning experience."
Gibbs' model transitions from objective reporting (Description) to subjective reflection (Feelings and Evaluation), culminating in critical thinking (Analysis). The "Action Plan" stage is particularly important - it requires specific, actionable steps. For instance, instead of vaguely noting "improve handovers", you might specify, "I will use the SBAR tool for all handovers starting tomorrow." This precision makes it especially useful for CPD portfolios, appraisals, and meeting revalidation standards.
To maximise its impact, reflect soon after clinical events and discuss your insights with colleagues. As Lucam Consultancy points out:
"Embracing this reflective model is a proactive step towards excellence in the dynamic field of healthcare."
Driscoll's What? So What? Now What? Framework
For those working in fast-paced environments, Driscoll's model offers a simpler alternative to Gibbs. Its three stages - What? (describe the event), So What? (analyse its importance), and Now What? (plan future actions) - allow for quick yet meaningful reflection.
This framework ensures that clinical experiences don't remain as vague thoughts but instead lead to actionable learning. For example, after a challenging patient interaction, you might ask yourself: What happened? Why does it matter? What will I do differently next time?
Despite its simplicity, the model still demands honest evaluation and clear action planning. Its straightforward structure respects the time constraints often faced by healthcare professionals while still promoting meaningful growth.
Kolb's Experiential Learning Cycle
David Kolb's model takes a dynamic approach, turning experiences into actionable learning. His four-stage cycle - Concrete Experience, Reflective Observation, Abstract Conceptualisation, and Active Experimentation - emphasises that learning comes from doing and reflecting, not just absorbing information. This approach is particularly effective for CPD planning and deeper learning.
The "Reflective Observation" stage encourages professionals to consider how their experiences align or conflict with prior knowledge and biases. "Abstract Conceptualisation" then helps refine or create new mental models, which can be applied across different clinical scenarios. Finally, "Active Experimentation" involves testing new approaches, ensuring that insights lead to better patient care.
Kolb also identifies four learning styles based on two continuums: Doing versus Watching (Active Experimentation vs Reflective Observation) and Thinking versus Feeling (Abstract Conceptualisation vs Concrete Experience). Understanding your learning style can help you strike a balance. For instance, if you’re naturally hands-on, make time for reading and research to ensure your decisions are evidence-based.
As ReflectRN explains:
"Reflection isn't about being self-critical. It's about being honest, open, and proactive in your learning."
Kolb's model ensures that learning is comprehensive, with all four stages contributing to skill development. Documenting completed cycles can also demonstrate how specific patient encounters have led to improvements in practice, supporting revalidation efforts.
Practical Ways to Build Reflective Practice Into Your Routine
Incorporating reflection into your daily clinical routine doesn’t have to be time-consuming. With just 15–20 minutes a day, you can create a habit that fits into even the busiest schedules. The secret lies in consistency - short, regular reflections are often more effective than sporadic, lengthy sessions.
Daily Reflection Habits
A straightforward "look back" routine at the end of your shift can turn scattered thoughts into meaningful insights. Ask yourself key questions like: What happened? What went well? What exceeded expectations? What feelings arose and why? What could have been done differently? What could be improved?.
For an even quicker approach, try the 3-2-1 method: jot down three observations, two questions, and one insight. Whether you use a notebook or a digital tool, the format is less important than making it a regular habit. As Stephen Brookfield puts it:
"Critical reflection is a tool to help us resist our habits and tendencies of justifying what we do by reference to unchecked 'common sense'."
Keeping a reflective journal can also be invaluable. A focused 500-word entry can help you uncover patterns, especially when dealing with situations that leave you feeling uncertain or uneasy. Sharing these reflections with colleagues can further enhance your understanding and learning.
Learning Through Peer Discussions
Reflection becomes even more meaningful when shared with others. For UK nurses and midwives, reflective discussions with another NMC registrant are a required part of revalidation. These discussions focus on written reflections and how they align with the professional Code. Your discussion partner could be a line manager, a regular colleague, or someone from your professional network - they don’t need to share your specialty or work environment.
Before these discussions, prepare written drafts using a structured model to guide the conversation. Whenever possible, hold these discussions face-to-face, using video calls only when necessary. Brian Lucas from The Open University highlights the value of this process:
"Reflection-on-action involves a retrospective critical exploration of an experience or incident to identify learning points".
This reflective process can happen one-on-one, during clinical supervision, or in group settings. If meeting in person isn’t an option, digital tools can help keep the process structured and effective.
Using Technology for Structured Reflection
Digital tools make structured reflection easier. Platforms like Reflection Guide offer step-by-step guidance using recognised models such as Gibbs, Driscoll, and Kolb. These tools can help you draft reflections suitable for NMC revalidation, HCPC CPD, or GMC appraisal. Built-in privacy features ensure that no patient information is accidentally included, which is crucial for portfolio submissions.
These platforms also allow you to export ready-made drafts, saving valuable time when preparing for revalidation, where five written reflections are required over a three-year period. Mobile apps can further support "reflection-in-action" by letting you capture clinical observations and insights immediately. This way, you can document experiences while they’re still fresh, avoiding the challenge of piecing events together later.
Overcoming Common Barriers to Reflection
Even when professionals recognise the importance of reflection, several obstacles can make it hard to engage in the process. Time pressures and workplace culture are often the biggest hurdles. Heavy workloads leave little room for reflection, and without management support, there’s often a lack of encouragement or dedicated time to practise it.
Emotional challenges also play a significant role. Reflection requires self-awareness and a willingness to confront emotions, which can feel overwhelming after a tough shift. Many professionals are reluctant to revisit stressful situations or worry they’re “doing it wrong” when they first start. As Cambridge University Libraries points out:
"Doing proper reflection takes time but you need to think of this as an investment in your education, your professional development and your own mental wellbeing".
Common Obstacles to Reflection
The barriers to reflection generally fall into three main categories: practical, cultural, and emotional.
- Practical barriers: Finding a quiet, suitable space for reflection can be a challenge, especially in busy clinical environments.
- Cultural barriers: If leadership doesn’t prioritise reflection, it can be hard for professionals to justify setting aside time for it. A workplace culture that values and supports reflection can make all the difference.
- Emotional barriers: Revisiting difficult clinical encounters can be emotionally draining, particularly after demanding shifts. This emotional toll often discourages professionals from engaging in reflective practices.
Understanding these challenges is the first step towards addressing them effectively.
How to Make Reflection a Consistent Practice
Once you’ve identified the barriers, there are practical strategies to help you build reflection into your routine. Start by creating a consistent habit. For example, set aside a regular time slot - such as the last 30 minutes of your day - for uninterrupted reflection. To stay focused, turn off notifications, step away from your usual workspace, and use tools like automated prompts or reminders. Even something as simple as a Post-it note can serve as a helpful nudge.
Don’t feel limited to a single reflective framework. Explore different models - like Gibbs, Driscoll, or Kolb - to find one that fits your style of thinking. Reflection doesn’t have to be a solo activity either; using clinical supervision sessions to reflect with a mentor or colleague can turn routine meetings into valuable opportunities. When discussing reflection with management, emphasising its benefits for staff performance and patient care can help secure their support.
Integrating reflection into your daily routine not only enhances your performance but also prepares you for long-term career growth.
Connecting Reflection to Career Development
For professionals in the UK, reflective practice is not just encouraged - it’s required for registration and revalidation. Beyond fulfilling these obligations, regular reflection can be a powerful tool for career advancement. As Becky Ingham-Broomfield, Casual Academic, explains:
"The use of an appropriate reflective model can assist nurses with self-improvement and personal development, while documenting the reflection process may help to develop their self-awareness".
Keeping a record of your reflections can serve as concrete evidence of your growth, whether for appraisals, job applications, or promotion discussions. Tools like Reflection Guide offer structured templates and modules that align with professional body requirements, making it easier to document your journey. Over time, maintaining a portfolio of reflections showcases not just your achievements, but how you’ve adapted, learned, and evolved as a healthcare professional.
Conclusion: Making Reflective Practice Part of Your Professional Life
Key Points for Healthcare Professionals
Reflective practice goes beyond being just a regulatory obligation - it's a meaningful way to foster continuous learning, personal growth, and emotional wellbeing. It has a direct impact on patient safety and strengthens teamwork by fostering shared understanding. Engaging in both "reflecting in practice" (adapting intuitively during events) and "reflecting on practice" (analysing experiences afterwards) helps build self-awareness and emotional intelligence. This approach allows you to turn workplace stress into constructive emotions, develop resilience, and reinforce your professional identity by aligning actions with your values and beliefs. Moreover, it enhances patient care by translating challenging situations into actionable improvements.
When you integrate reflective practice into your routine, you not only meet professional standards but also elevate your clinical expertise. This mindset prepares you to apply these concepts practically in your daily work.
Start Reflecting Today
The benefits are clear - so why wait? Begin incorporating reflection into your routine right away. A simple starting point is the 3-2-1 method: jot down three observations, two questions, and one insight each day. Use brief moments, like your commute, to reflect on recent experiences while they're still fresh. Focus on specific critical incidents - whether successes or challenges - rather than reflecting on every minor task, as this can lead to burnout.
To make the process easier, tools like Reflection Guide offer structured templates and modules designed to align with professional body requirements. These tools help you maintain a reflective diary and track your progress over time. Keep in mind the "4 Cs" of effective reflection: it should be Continuous, Connected, Challenging, and Contextualised. By turning reflection into a regular habit rather than a box-ticking exercise, you'll unlock its full potential for improving both your career and overall wellbeing.
FAQs
How do I know I’m reflecting properly?
Reflecting effectively requires an approach that's deliberate, thoughtful, and continuous. It's about delving into your experiences, actions, emotions, and decisions, while taking a critical look at your strengths, areas for improvement, and chances to develop further. Tools like the 5 Rs framework - reacting, recording, reviewing, revising, and reworking - can provide a clear structure to guide this process.
In healthcare, reflection isn't just a personal exercise; it plays a key role in fostering both personal and professional development. It helps practitioners align with professional standards, refine their practice, and enhance their overall wellbeing.
Which reflective model should I use for my situation?
The most suitable reflective model often hinges on what you need it for and the situation you're in. Gibbs’ Reflective Cycle is a more structured option, perfect for in-depth analysis, as it guides you through each step methodically. On the other hand, Driscoll’s model keeps things straightforward, making it a handy choice for quick reflections. If you're aiming for experiential learning or advancing professionally, Kolb’s cycle is a solid pick. In healthcare, many professionals lean towards Gibbs’ model because its detailed framework is particularly useful for revalidation and refining future practices.
How can I reflect without breaching patient confidentiality?
To reflect effectively on clinical practice while safeguarding patient confidentiality, shift the focus to your own actions, emotions, and lessons learned. Avoid sharing identifiable details like names, dates, or unique case characteristics. Instead, use generalised scenarios or anonymised descriptions. This method allows you to engage in meaningful professional reflection while ensuring patient privacy remains intact.
