How to Write a Reflective Essay for Nursing Students

Writing a reflective essay is an essential skill for nursing students. Not only does it help you meet academic and professional requirements, but it also supports personal and professional growth. Reflective essays are especially important for meeting the Nursing and Midwifery Council (NMC) revalidation standards in the UK. Here's what you need to know:
- Purpose of Reflective Essays: They connect clinical practice to professional standards like "The Code", which includes prioritising people, practising effectively, preserving safety, and promoting professionalism.
- Choosing the Right Experience: Focus on clinical moments that challenged you emotionally or professionally, such as ethical dilemmas, communication breakdowns, or knowledge gaps.
- Using Reflective Models: Frameworks like Gibbs Reflective Cycle, Driscoll Model, and Kolb’s Experiential Learning Cycle help structure your essay.
- Key Steps: Start with a concise introduction, describe the event briefly, analyse its significance, share your emotions, and create a clear action plan using SMART goals.
- Avoid Common Mistakes: Keep descriptions brief, focus on analysis, maintain confidentiality, and link your reflection to NMC standards.
Reflective writing isn't just an academic exercise - it’s a vital tool for improving patient care and developing your skills as a nurse. Follow these steps to craft a meaningful and professional reflective essay.
Choosing a Clinical Experience to Reflect On
How to Identify Key Experiences
Picking the right clinical experience is crucial for writing a reflective essay that not only supports your professional growth but also meets NMC revalidation requirements.
Look for experiences that pushed you out of your comfort zone or challenged your perspective. Focus on moments where strong emotions - like powerlessness, embarrassment, compassion, or even surprise - came into play. These situations often serve as powerful catalysts for self-awareness and professional development.
Adverse events, such as communication breakdowns or medical errors, can also provide valuable learning opportunities. For instance, one student at an NHS teaching hospital reflected on their first clinical posting, where they felt "embarrassed" and "silent" when a patient asked about influenza, and they didn’t know the answer. This moment of vulnerability highlighted the gap between theoretical knowledge and practical application, sparking meaningful reflection on their readiness for clinical practice.
As you review your clinical hours, ask yourself: Which moments made me question my approach? When did I feel tested in my knowledge or skills? These could include scenarios involving ethical dilemmas, teamwork challenges, or times when you felt unprepared. For example, another student reflected on a "communication dilemma" involving a diabetic patient facing leg amputation. The lack of compassion shown by the surgical team left the student feeling powerless to provide emotional support, making it a profound learning experience.
Lastly, ensure the experience you choose aligns with the NMC standards for reflective practice.
Aligning Your Experience with NMC Requirements
Your chosen experience should directly link to one or more key themes of the NMC Code: Prioritise people, Practise effectively, Preserve safety, or Promote professionalism and trust. The Royal College of Nursing emphasises this by stating:
Any reflective account needs to explain what you learnt from the CPD activity, feedback or experience; how you changed or improved your work as a result, and how this is relevant to the Code.
When selecting your scenario, ensure it allows you to address all three aspects: what you learned, how your practice evolved, and how it ties back to professional standards. Protect patient and staff confidentiality by removing any identifying details. Keep the focus on your personal learning journey, providing enough depth to meet the requirements of your assignment or revalidation.
sbb-itb-a476a38
How to write a reflection for an assignment | Nursing UK
Reflective Models for Nursing Students
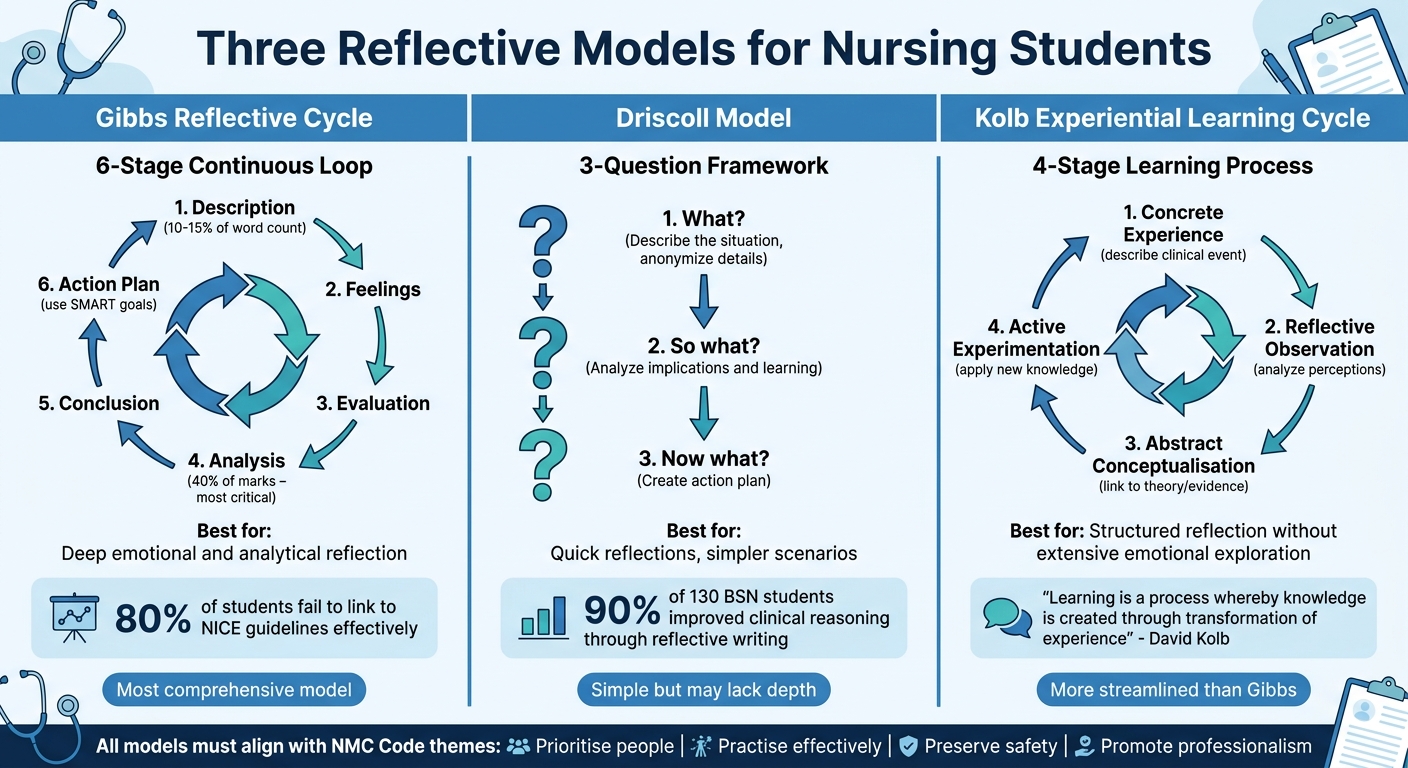
Comparison of Three Reflective Models for Nursing Students: Gibbs, Driscoll, and Kolb
Reflective models help nursing students turn clinical experiences into meaningful learning opportunities. Instead of writing a scattered account of events, these models provide a structured method that meets academic expectations and the Nursing and Midwifery Council (NMC) guidelines. They guide you through a clear process to ensure all critical elements of reflection are addressed.
Three of the most commonly used models in nursing education are Gibbs Reflective Cycle, Driscoll Model of Reflection, and Kolb Experiential Learning Cycle. Each offers a unique framework, but all aim to help you critically analyse your experiences and create actionable plans for professional development. The choice of model depends on the depth of analysis and the complexity of the experience you're reflecting on.
Gibbs Reflective Cycle
Gibbs Reflective Cycle is a six-stage process designed to encourage continuous learning. The stages include Description, Feelings, Evaluation, Analysis, Conclusion, and Action Plan. It’s not a simple checklist but an ongoing loop that accommodates both emotional and analytical aspects of reflection.
When writing the Description, stick to the facts - who was involved, what happened, and where it took place. This section should only take up about 10–15% of your word count.
The Analysis stage is often the most challenging but also the most critical, as it usually accounts for up to 40% of the marks in nursing assignments. This is where you connect your experience to academic research and evidence-based practices. Many students struggle to link their reflections to NICE guidelines, with 80% failing to do so effectively. Addressing this gap can make your work stand out. As Neelam Hussain, a Senior NHS Sister and Clinical Competency Lead, explains:
Reflection is not just a university requirement; it is a professional safeguard. The goal is to bridge the gap between clinical theory and safer patient outcomes.
For the Action Plan, use SMART goals (Specific, Measurable, Achievable, Realistic, Time-bound). For example, you might set a goal like: Complete the Trust's SBAR training by 15th June 2026 and participate in three supervised handovers. This ensures your reflection meets both NMC and professional standards.
Driscoll Model of Reflection
The Driscoll Model simplifies the reflection process into three straightforward questions: What?, So what?, and Now what?. This approach, based on Terry Borton’s framework, is ideal for quick reflections but may not allow for in-depth analysis.
- What? focuses on describing the situation, including the context, your role, and your initial feelings. Ensure patient details are anonymised to maintain professional standards.
- So what? involves analysing the implications of the event. Discuss your thoughts, the knowledge you applied, and what the experience taught you about your practice.
- Now what? is about creating an action plan. Identify what needs to change, what training you require, and how you’ll approach similar situations in the future.
The University of Edinburgh’s Reflection Toolkit highlights:
The simplicity of this model is both a great strength and a possible limitation.
To avoid shallow reflections, break each stage into sub-questions. For instance, under "What?", ask: What was I trying to achieve? or What were the consequences for the patient? In the "Now what?" stage, link your planned actions to professional standards.
A study involving 130 BSN students found that reflective writing improved clinical reasoning in 90% of participants. This demonstrates how structured reflection can enhance professional practice.
Kolb Experiential Learning Cycle
Kolb’s cycle offers a dynamic way to turn experiences into actionable improvements. It defines learning as a process of creating knowledge through the transformation of experience. The cycle includes four stages: Concrete Experience, Reflective Observation, Abstract Conceptualisation, and Active Experimentation.
- Concrete Experience focuses on describing a specific clinical event, including factual details, your role, and the environment.
- Reflective Observation involves analysing what you observed and how your perceptions or feelings evolved during the experience. Use this stage to identify patterns in your behaviour by comparing it to past events.
- Abstract Conceptualisation is where you develop new ideas or theories based on the experience, linking it to broader nursing concepts or evidence-based practices. Clearly state how the experience aligns with professional standards.
- Active Experimentation outlines how you’ll apply your new knowledge in practice to improve patient care.
Kolb’s model is more streamlined than Gibbs, making it a good option when you need structure but don’t require extensive emotional exploration. As David Kolb noted:
Learning is a process whereby knowledge is created through a transformation of experience.
This approach ensures your reflective writing supports both professional growth and compliance with NMC standards.
How to Write a Reflective Essay: Step-by-Step
Writing a reflective essay doesn't have to feel overwhelming. Once you've selected a reflective model to guide your work, the process becomes much simpler when broken down into manageable steps. The goal is to move from describing an event to evaluating its significance and planning for future growth. Each step builds upon the last, creating a structured narrative that highlights your professional development.
Step 1: Write the Introduction and Describe the Experience
Your introduction is your chance to set the stage for the essay. Start with a clear purpose and mention the reflective model you'll be using. For example: "This reflection uses Gibbs' Reflective Cycle to examine a medication administration incident during my placement on a medical ward." Also, include a confidentiality statement early on, such as: "In accordance with the NMC Code regarding confidentiality, the patient will be referred to as 'Patient A'".
A strong introduction grabs attention, explains your essay's purpose, previews key themes, and presents a concise thesis. For instance, you might outline themes like communication barriers, teamwork, or specific clinical skills.
When describing the event, stick to the facts and present them in chronological order. Focus on the "what, where, who, and how", but avoid analysing the situation at this stage. This section should take up only 10–15% of your total word count. Use past tense to recount events (e.g., "I noticed", "The patient said"). As John Launer explains:
The act of writing itself creates new and original ideas. By recalling an event, slowing it down in your mind, and anatomising it in writing, you can deepen your understanding of it.
Step 2: Share Your Emotions and Thoughts
Reflective essays encourage self-awareness, so clearly express your emotional responses to the experience. Whether you felt anxious, confident, or uncertain, sharing these emotions helps explain your actions. For instance, you could write: "I felt uncertain about escalating the patient's deteriorating observations because I worried about appearing incompetent in front of senior staff."
Acknowledging discomfort or mistakes is essential for growth, but maintain a professional tone throughout. Use first-person pronouns freely, as this style of writing allows for personal reflection.
Think about how your emotions changed during and after the event. Did initial anxiety shift to confidence after receiving support? Did confusion give way to clarity after discussing the incident with a mentor? Documenting these changes adds depth and sets the stage for the next step: analysing the experience.
Step 3: Analyse and Evaluate the Experience
This is where you dig deeper, moving beyond description to explore the "why" behind the event. Consider factors like communication styles, workplace culture, existing policies, or your own knowledge gaps. This analysis connects your personal feelings to the broader clinical challenges you encountered.
A balanced evaluation looks at both successes and areas for improvement. For example, you might acknowledge that you correctly identified a patient's deteriorating condition but struggled to communicate this effectively using SBAR (Situation, Background, Assessment, Recommendation). Strengthen your analysis by linking it to evidence-based guidelines.
Brian Lucas, Associate Lecturer at The Open University, highlights the importance of this process:
Reflection is a vital element of nursing practice and has a wide-ranging purpose including, for example, self-inquiry into experiences to find meaning, gain insight and prompt action.
Explain how your understanding evolved. Perhaps you initially thought the issue was purely clinical, but later realised it involved systemic communication failures. This kind of critical thinking enriches your reflection.
Step 4: Develop Conclusions and an Action Plan
Conclude by identifying what you’ve learned and outlining a clear action plan. Reflect on how this experience will shape your future practice.
Your action plan should follow SMART goals (Specific, Measurable, Achievable, Realistic, Time-bound). For example: "Complete the Trust's SBAR training by 15th June 2026 and participate in three supervised handovers with my mentor by 30th June 2026."
If your reflection identified a knowledge gap - such as recognising sepsis - include steps to address it, like reviewing Sepsis Trust guidelines or attending mandatory training. Detail both short-term actions and longer-term development goals.
Step 5: Align with NMC Standards and Write the Conclusion
Link your reflection to the NMC Code, which outlines four key themes: Prioritise people, Practise effectively, Preserve safety, and Promote professionalism and trust. Ask yourself questions like, "How does this activity relate to the NMC Code?" and "What have I learned that enhances my professional competence?".
Be specific. If your experience involved advocating for a patient with communication difficulties, connect it to "Prioritise people" by explaining how you ensured their voice was heard in care planning. If a medication error occurred, relate it to "Preserve safety" by describing how you reported the incident.
The Royal College of Nursing defines reflection as:
A conscious effort to think about an activity or incident that allows us to consider what was positive or challenging and, if appropriate, plan how it might be enhanced, improved or done differently in the future.
Summarise the lessons learned and highlight how the experience has shaped your professional identity. Emphasise the impact on patient care and your commitment to evidence-based practice. This final step transforms your reflection into a tool for improving both your skills and patient outcomes.
Common Mistakes and How to Avoid Them
Even with a well-structured reflective model, nursing students can stumble into common pitfalls that affect the quality of their reflections. These include providing excessive detail about events, leaning too much on storytelling instead of analysis, drafting unclear action plans, and failing to maintain confidentiality.
Balancing Description and Analysis
One frequent issue is spending too much time describing events. Some students dedicate over half of their essay to narration, leaving little room for the crucial analysis that demonstrates actual learning. Ideally, the event description should take up only 10–15% of your total word count. The bulk of your reflection should be focused on evaluation, analysis, and planning for your future development.
Here’s the key: your assessor already knows how standard clinical procedures work. What they’re looking for is your ability to critically analyse the experience and connect it to professional standards. For example, instead of writing several paragraphs on how you prepared medications, briefly summarise the steps, then dive into why communication with the patient may have faltered or how your understanding of pharmacology guided your actions.
Neelam Hussain, Senior NHS Sister and Clinical Competency Lead, highlights this point:
Reflection is not just a university requirement; it is a professional safeguard. The goal is to bridge the gap between clinical theory and safer patient outcomes.
Ground your emotions in theory rather than just stating them. Instead of saying, "I felt anxious", explain how that anxiety influenced your clinical judgement or objectivity, perhaps referencing frameworks like Peplau's Theory of Interpersonal Relations. Keep in mind that analysis often accounts for up to 40% of your marks, so focus on depth rather than excessive detail.
Maintaining Honesty and Professionalism
Once you’ve balanced your narrative, it’s essential to ensure your reflection remains professional. Honest self-assessment is vital, but it should always be framed constructively. Use formal language and thoughtful self-criticism. Acknowledging discomfort or mistakes shows self-awareness, but make sure to present these in a way that highlights your learning.
Avoid vague statements like "I’ll try to be more careful next time." Instead, set clear, actionable goals. For instance, you might commit to completing a Trust-certified workshop within 30 days or arranging three supervised practice sessions with your mentor.
Another misstep is suggesting that an experience or feedback didn’t influence your practice. Even if an event confirmed your existing knowledge, discuss how it reinforced your confidence or highlighted a key skill. Your reflection should always demonstrate growth or insight.
And, of course, protecting patient information is non-negotiable.
Protecting Patient Confidentiality
Breaching confidentiality is one of the most serious errors you can make. This isn’t just about maintaining trust; it’s a regulatory requirement. Including identifiable patient or staff details could lead to an automatic "Fitness to Practice" referral. The NMC Code explicitly requires maintaining confidentiality as part of its commitment to "Prioritise people" and "Promote professionalism and trust."
Ensure all patient identifiers are anonymised. For example, you might write: "In accordance with the NMC Code regarding confidentiality, the patient will be referred to as 'Patient A'". Use general descriptions, such as "a patient in their 60s", rather than specific ages, dates, or unique identifiers.
Perform a thorough check to remove any details like ward names, dates, or other identifiable information. As the Nursing and Midwifery Council advises:
Be careful not to record any information which may identify another person.
Your description should be clear enough to support your reflection but vague enough to protect identities. Focus on your actions, learning, and development, ensuring compliance with data protection laws while still delivering a meaningful reflection.
Conclusion
The Role of Reflection in Nursing Practice
Reflective writing isn't just a tick-box exercise or academic task; it's a critical tool for bridging the gap between theoretical knowledge and safer patient care. For instance, the Nursing and Midwifery Council (NMC) mandates five reflective accounts every three years as part of revalidation. This process helps identify areas for improvement by drawing lessons from CPD activities, feedback, or clinical scenarios. Reflection also nurtures self-awareness, which strengthens leadership skills, builds confidence, and bolsters resilience. By linking your reflections to the NMC Code's themes, you ensure alignment with professional standards while enhancing patient outcomes.
Final Tips for Writing a Reflective Essay
To make your reflective essay impactful, consider these practical strategies:
- Keep event descriptions concise - limit them to 10–15% of your word count. This leaves ample space for critical analysis, which can account for up to 40% of your marks. Focus on extracting meaningful insights rather than recounting events.
- Write in the first person using "I" and "me" to convey your personal experiences and emotions. Honest reflections on mistakes or challenges show professional growth and a deep commitment to learning.
- Always anonymise patient information by using pseudonyms like "Patient A" to maintain confidentiality.
When crafting your action plan, ensure it follows the SMART framework: Specific, Measurable, Achievable, Realistic, and Time-bound. Avoid vague goals like "I'll try harder", and instead focus on clear, measurable steps that demonstrate a commitment to improvement.
Make use of the NMC's reflective accounts form and consider incorporating reflection into your weekly routine. As the NMC emphasises:
We want to encourage nurses, midwives and nursing associates to reflect on their practice, so they can identify any improvements or changes to their practice as a result of what they have learnt.
FAQs
How do I choose a good clinical experience to reflect on?
During a recent shift, I encountered a situation that deeply impacted my professional growth and understanding of patient care. A middle-aged patient with advanced COPD (Chronic Obstructive Pulmonary Disease) was admitted, struggling with severe breathlessness and anxiety. While managing the physical symptoms was a priority, it quickly became apparent that the emotional toll of their condition required equal attention.
As I approached the patient, their visible distress made communication challenging. I decided to take a step back, sit beside them, and speak in a calm, reassuring tone. I encouraged them to focus on their breathing while I guided them through relaxation techniques. This small but intentional act seemed to ease their anxiety, allowing us to proceed with the necessary medical interventions.
What struck me most about this interaction was the importance of holistic care. While I was initially focused on the clinical management of their condition, this experience reminded me that addressing emotional needs is just as critical. It reinforced the value of empathy, patience, and active listening in building trust and providing effective care.
Reflecting on this moment, I realised how vital it is to adapt my approach based on the unique needs of each patient. It also highlighted the significance of continuous learning, as I later researched more about managing anxiety in patients with chronic illnesses. This experience aligns closely with the NMC Code, particularly in prioritising people and practising effectively, and has motivated me to explore further training in psychological support techniques.
This interaction not only challenged me to think critically about my practice but also emphasised the profound impact of compassionate care. It’s a reminder that even in high-pressure situations, taking the time to connect with patients on a human level can lead to better outcomes for everyone involved.
Which reflective model should I use for my nursing essay?
When it comes to reflective writing in nursing, the choice of model often depends on what suits your specific needs. Three commonly used frameworks are Gibbs' Reflective Cycle, Driscoll's Model of Reflection, and Kolb's Experiential Learning Cycle. These models provide a structured approach to reflection by helping you:
- Describe the event: What happened?
- Analyse the situation: Why did it happen? What went well or poorly?
- Identify lessons learned: What have you gained from the experience?
- Plan future actions: How will you apply this knowledge going forward?
It's important to select a model that not only meets the Nursing and Midwifery Council (NMC) requirements but also clearly showcases your professional development and learning journey.
How can I include enough detail without breaching confidentiality?
When writing a reflective essay, it's crucial to include enough detail to make your experiences and insights clear, but without compromising confidentiality. Avoid mentioning identifiable information such as names, specific locations, or any unique personal details. Instead, keep descriptions general and factual, ensuring they are anonymised. Concentrate on your professional actions, decisions, and the lessons you’ve learned. This approach allows for meaningful reflection while staying within confidentiality guidelines.
